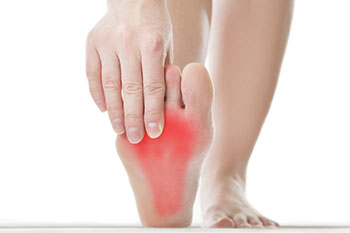
Plantar fasciitis is a condition in which the plantar fascia, the ligament that runs along the bottom of the foot and connects the toes to the heel bone, becomes inflamed. This most often occurs due to overuse, or repetitively doing activities that put excessive strain on the plantar fascia. Unsurprisingly, plantar fasciitis is a common injury among runners and other athletes. Other possible causes for plantar fasciitis include wearing unsupportive shoes and standing for prolonged periods of time. People who are obese, have flat feet, abnormally high arches, or are pregnant may be at an increased risk of developing this condition.
The telltale symptom of plantar fasciitis is an acute, sharp, stabbing pain in the heel. This pain may radiate to the arch of the foot, and you may also notice swelling near the heel. The pain is usually at its worst when you take your first few steps after a long period of rest, such as when you get out of bed in the morning. As you walk, the pain may subside, but can reemerge after spending a long period of time on your feet. Without treatment, the pain may gradually increase over a period of several months and become chronic.
Treatment for plantar fasciitis is usually conservative and begins with resting and icing the affected foot, stretching, taking anti-inflammatory medications, and wearing comfortable and supportive shoes. If the pain persists, your doctor may suggest padding, taping, or strapping the affected foot, wearing orthotics, a night splint, or a cast, corticosteroid injections into the foot, and physical therapy. If these treatment methods do not produce results, surgery can be considered.
If you are experiencing the symptoms of plantar fasciitis, please seek the care of a podiatrist.
